

Vaccines prevent disease by providing acquired immunity. Read the overview below to gain an understanding of vaccination and explore the previews of articles examining differing perspectives on vaccination.
Weidman Burke, Chelsea. "Vaccination." Gale Health and Wellness Online Collection, Gale, 2021.
Vaccines protect you (and everyone around you) from highly infectious and potentially deadly pathogens (disease-causing organisms such as bacteria and viruses) without you needing to be exposed to the actual pathogen. Medical historians consider vaccines one of the most important advances in medicine, and vaccines save the lives of millions of people around the globe each year.
Vaccines allow your body to produce infection-fighting cells and pathogen-specific antibodies, which are the molecules that remain in your immune system and recognize and attack pathogens. A vaccine mimics an infection by exposing your immune system to a weakened or dead pathogen, allowing the system to recognize this pathogen and build up protection against it. Then, if you are exposed to the real pathogen, you are protected, or at least much less likely to acquire that particular disease and experience complications from it.
It takes up to two weeks for you to be fully protected after getting a vaccine because it takes that long for pathogen-specific antibodies to be produced. If you are exposed to a pathogen before or right after getting the vaccine for it, you may get sick simply because your immune system hasn't had time to produce enough antibodies.
You may have minor symptoms after getting a vaccine, such as aches and fever, that feel like you're getting sick, but you aren't (vaccines almost never cause the illness they aim to protect you from). The symptoms you feel are your immune system responding to the vaccine and producing protection against the pathogen.
What is herd immunity (community immunity)?
Vaccination not only protects yourself, it also protects everyone around you. If enough people get vaccinated (between 75–94% of the population, depending on the disease), it will likely protect those who don't get vaccinated. When enough people are vaccinated against the disease, a pathogen has a hard time being passed from person to person and can't spread easily through a community.
Herd immunity is especially important to those who can't get vaccinated because they are too young, too old, too sick, or have an allergy or chronic condition that prevents them from receiving a specific vaccine. It can even protect the few people who have been vaccinated but didn't have a strong immune response to them, leaving them vulnerable to disease.
Protecting yourself and your community aren't the only reasons to vaccinate. As more people in a region vaccinate, the diseases they protect against become rarer; in fact, if the vast majority of people immunize for long enough, diseases can be eradicated from their region. Smallpox, for example, was eradicated worldwide.
On the flip side, if we stop vaccinating, we make ourselves and our communities much more vulnerable to diseases and epidemics.
Like any medicine, vaccines can cause side effects, but they are usually mild (low-grade fever, sore throat, soreness around the injection site) and go away a few days after getting vaccinated. However, there is an extremely small chance you could have a more serious rare side effect, such as a severe allergic reaction, other serious injury, or death.
There is a one in a million chance of having a serious reaction to a vaccine, according to the Centers for Disease Control and Prevention (CDC). The risks and complications associated with many of the serious diseases that vaccines protect against have much higher odds of causing problems if you were to get sick with them.
Outbreaks can happen when people hesitate or refuse to vaccinate themselves or their kids (usually called being "vaccine hesitant" or "anti-vax"). When an entire community has low enough vaccination rates, outbreaks can occur because the pathogen can circulate, spreading from person to person.
An infamous anti-vax example involves the measles, mumps, and rubella (MMR) vaccine. The false link between MMR vaccination in children and the development of autism was made by discredited former British doctor Andrew Wakefield in a now retracted Lancet article published in 1998. But the damage was done; its publication sparked a large multinational anti-vax movement that has lowered immunity coverage in certain areas, which act as breeding grounds for recent measles outbreaks.
Since that infamous paper was published, researchers have studied the possible link between MMR vaccination and autism in millions of children around the world in multiple large-scale clinical studies. One such recent study look at over 657,000 children in Denmark born between 1999 through December 31, 2010. MMR vaccination was not found to increase the risk for autism, even in children susceptible to autism (those who had a sibling with autism or other autism risk factors). This adds even more evidence to support other large-scale studies that also did not find a connection between MMR vaccination and autism.
The World Health Organization declared the anti-vaccine movement as one of the top ten threats to global human health in 2019.
Developing a vaccine against a pathogen depends on multiple factors, such as if it is a bacteria or virus, what part of it is infectious, and how the immune system responds to it. Therefore, there are many different kinds of vaccines:
There are vaccines for over 20 different bacteria and viruses, with some vaccines having multiple different types, formulations, and dosing schedules. To help organize when you should get which vaccine, the CDC publishes vaccine schedules for children and adults. The children and adolescent (from birth to 18 years old) vaccine schedule can be found here: https://www.cdc.gov/vaccines/schedules/hcp/imz/child-adolescent.html.
The adult (18 years and older) vaccine schedule can be found here: https://www.cdc.gov/vaccines/schedules/hcp/imz/adult.html.
In general, the majority of routine vaccines are recommended to infants between birth and 18 months because their immune systems are still forming and encountering new bacteria and viruses. The ideal situation is to have a child be vaccinated before they come in contact with the bacteria or virus so they are protected once they do encounter the pathogen.
Some vaccines require multiple doses to achieve the best protection possible due to a variety of factors, including the type of vaccine it is (inactivated vaccines, for example), not enough antibodies being produced after the first dose to successfully fight off an infection, or protection wearing off over time.
A few vaccines need to be regularly administered throughout adulthood to maintain protection, such as the annual flu shot or the tetanus shot booster every 10 years. The specific flu viruses that are most prevalent in a season tend to change from year to year, which is why you need to get a new flu shot each year.
Two vaccines, the shingles and pneumococcal shots, are recommended for people aged 65 and older because they are at a greater risk of both shingles and pneumococcal infections. The human papillomavirus (HPV), which is typically given to adolescents ages 11-12, has now been recommended for men and women up to age 45, especially if they were not adequately vaccinated when they were younger.
Some vaccines are only recommended if you are traveling to certain parts of the world where the diseases they protect against are common, such as yellow fever or typhoid.
People experiencing homelessness may also be recommended to receive an additional hepatitis A vaccination to prevent against infection or control outbreaks. People who use injection drugs should be vaccinated against hepatitis A and B and should be tested for hepatitis B and C.
Certain populations may have specific vaccination needs or altered recommendations, including those who are pregnant, health care professionals, men who have sex with men, are immunocompromised, or have certain medical conditions (HIV infection, heart or lung disease, diabetes, renal disease, chronic liver disease, or asplenia). The complete altered vaccination schedule can be found here: https://www.cdc.gov/vaccines/schedules/downloads/adult/adult-combined-schedule.pdf.
Websites
"The Advisory Committee on Immunization Practices' Interim Recommendation for Allocating Initial Supplies of COVID-19
Vaccine—United States, 2020." Centers for Disease Control and Prevention. December 11, 2020. https://www.cdc.gov/mmwr/volumes/69/wr/mm6949e1.htm (accessed March 26, 2021).
Hviid, Anders, et al. "Measles, Mumps, Rubella Vaccination and Autism: A Nationwide Cohort Study." Annals of Internal Medicine. April 16, 2019. https://www.acpjournals.org/doi/10.7326/M18-2101 (accessed March 26, 2021).
"Table 1. Recommended Adult Immunization Schedule for ages 19 years or older, United States, 2021." Centers for Disease Control and Prevention. February 12, 2021. https://www.cdc.gov/vaccines/schedules/hcp/imz/adult.html (accessed March 26, 2021).
"Table 1. Recommended Child and Adolescent Immunization Schedule for ages 18 years or younger, United States, 2021." Centers for Disease Control and Prevention. February 12, 2021. https://www.cdc.gov/vaccines/schedules/hcp/imz/child-adolescent.html (accessed March 26, 2021).
"Understanding How Vaccines Work." Centers for Disease Control and Prevention. July 2018. https://www.cdc.gov/vaccines/hcp/conversations/downloads/vacsafe-understand-color-office.pdf (accessed March 26, 2021).
"Vaccine Basics." Vaccines.gov. March 2020. https://www.vaccines.gov/basics (accessed March 26, 2021). "Vaccine Information Statements (VISs)." Centers for Disease Control and Prevention. April 1, 2020. https://www.cdc.gov/vaccines/hcp/vis/index.html (accessed March 26, 2021).
Organizations
Advisory Committee on Immunization Practices (ACIP), Centers for Disease Control and Prevention (CDC), 1600 Clifton Road, N.E., Mailstop H24-8, Atlanta, GA, 30329-4027, [email protected], www.cdc.gov/vaccines/acip/index.html.
Centers for Disease Control and Prevention (CDC), 1600 Clifton Rd, Atlanta, GA, 30333, (800) CDC-INFO (232-4636), http://www.cdc.gov/cdc-info/requestform.htmlh, ttp://www.cdc.gov .
National Institute of Allergy and Infectious Diseases, National Institutes of Health, 5601 Fishers Ln, MSC 9806, Bethesda, MD, 20892-9806, (301) 496-5717, (866) 284-4107 or TDD (800) 877-8339 (for hearing impaired), Fax: (301) 402-3573, [email protected]h, ttps://www.niaid.nih.gov/ .
National Vaccine Program Office, Office of Infectious Disease and HIV/AIDS Policy, U.S. Department of Health & Human Services, 300 C St, SW, Room L001, Washington, DC, 20024, (202) 795-7697, Fax: (202) 691-2102, https://www.hhs.gov/vaccines/index.html.
Source Citation (MLA 9th Edition)
Weidman Burke, Chelsea. "Vaccination." Gale Health and Wellness Online Collection, Gale, 2021. Gale Health and Wellness, link.gale.com/apps/doc/KUEGUS719023164/HWRC?u=omni&sid=bookmark-HWRC&xid=a6b92ead. Accessed 23 June 2022.
Gale Document Number: GALE|KUEGUS719023164
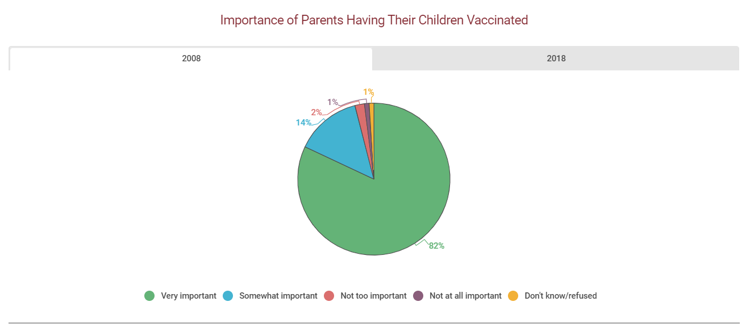
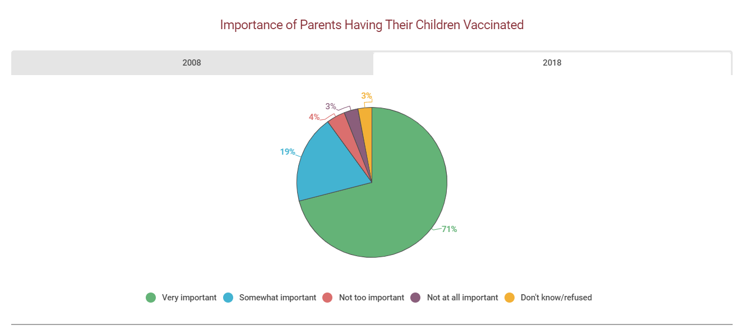
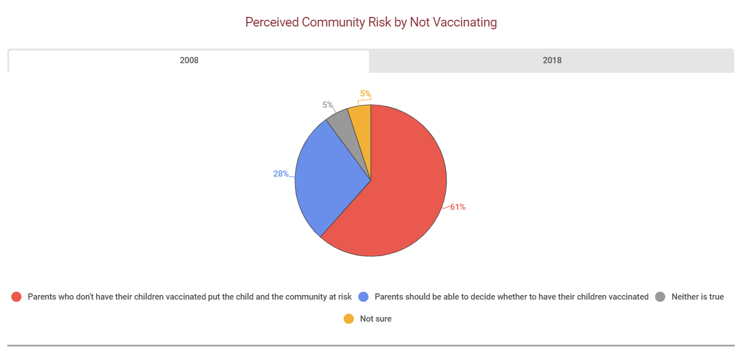
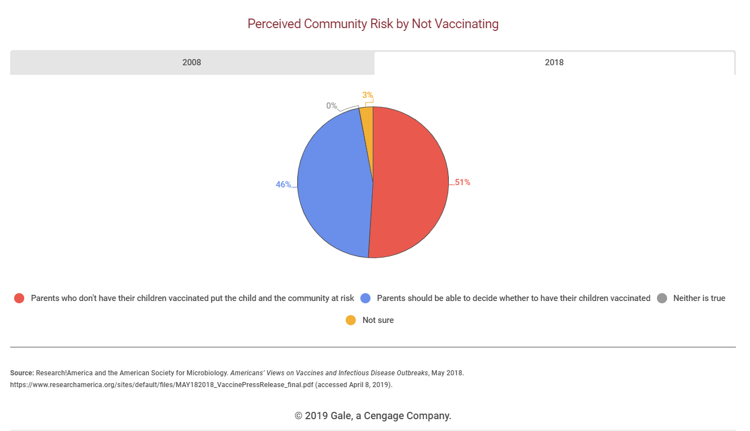
Source: "Academy of American Family Physicians, http://www.aafp.org. Disclaimer: This information is not a tool for self-diagnosis or a substitute for professional care. This image may be used for personal, non-commercial purposes only.
"US Public Opinion Regarding Childhood Vaccinations, 2008 and 2018." Gale Opposing Viewpoints Online Collection, Gale, 2019, www.gale.com.